



In a tropical climate like Kolkata, the transition into May brings a significant physiological shift for the skin. As the dew point rises, maintaining a professional summer skincare routine for humidity becomes essential to prevent follicular occlusion and inflammatory acne flares.
The transition from the dry spring months to the intense pre-monsoon heat of May presents a unique clinical challenge for residents of Kolkata. As ambient humidity levels frequently surpass 80%, the skin’s ability to regulate temperature through sweat evaporation is significantly impaired, leading to a phenomenon known as hyper-hydration of the keratin layer and subsequent pore blockage. To maintain a healthy acid mantle and prevent the onset of inflammatory acne, it is imperative to transition to a scientifically structured summer skincare routine for humidity. Unlike heavy winter regimens that rely on occlusive barriers, a professional skincare routine focuses on stabilising the Stratum Corneum using lightweight, humectant-based layering.
High ambient humidity directly alters the biophysical properties of the Stratum Corneum. While atmospheric moisture prevents traditional dryness, it introduces three specific clinical challenges that a summer skincare routine for humidity must address:
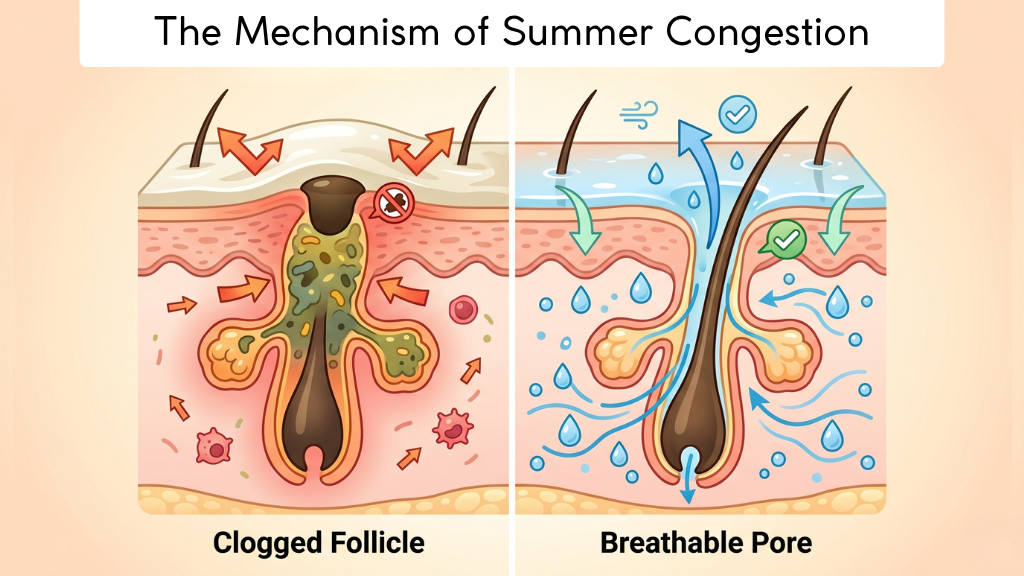
Many patients present with tiny, uniform bumps during April and May. This is often Acne Aestivalis, a condition triggered when UV radiation reacts with heavy, occlusive skincare ingredients. A standard winter regimen relies on occlusives (like petrolatum or heavy waxes) to prevent Transepidermal Water Loss (TEWL). However, in a summer skincare routine, these same ingredients act as a sealant that traps heat, sweat, and bacteria, leading to rapid follicular congestion.

To stabilize the skin barrier before the May heat peak, Wizderm recommends the following clinical protocol:
The first step in an effective summer skincare routine for humidity is the removal of oxidised lipids.
The “Skin Flooding” technique is a dermatological method of saturation using humectants rather than emollients.
A common mistake in a summer skincare routine for humidity is skipping moisturiser entirely, which leads to reactive seborrhea (overproduction of oil).
UV-induced inflammation is exacerbated by heat.
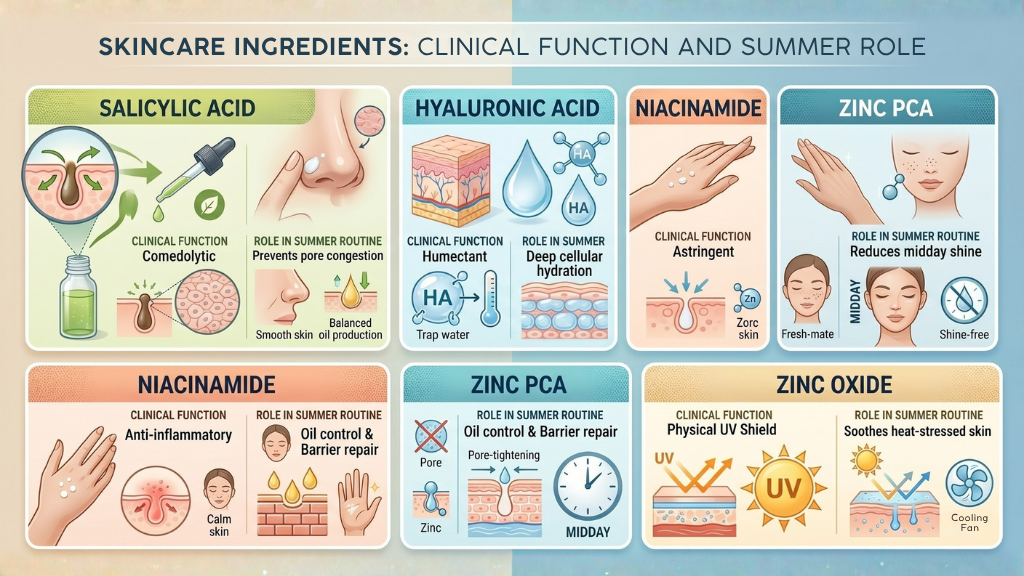
When a topical summer skincare routine for humidity is insufficient to manage persistent follicular congestion or Sebaceous Hyperplasia (enlarged oil glands), professional clinical intervention becomes necessary to reset the skin’s baseline. At Wizderm, we utilise medical-grade technologies that go beyond the surface to treat the root causes of summer skin distress.
While standard facials often rely on manual extractions that can cause micro-tears and inflammation, our Medical Hydra-Facial utilises patented Vortex-Fusion technology. This is the cornerstone of a clinical summer skincare routine for humidity.
The Mechanism: The procedure uses a specialized vacuum tip to create a localized “vortex” that dislodges “summer plugs”—a dense mixture of oxidized sebum, sweat, and atmospheric pollutants (PM2.5) that accumulate in Kolkata’s humid air.
The Infusion: Once the pores are evacuated, the device performs “Hydroporation,” forcing a cocktail of low-molecular-weight Hyaluronic Acid, Salicylates, and Peptides into the dermis.
Clinical Benefit: This provides a “Skin Flood” at a depth that topical serums cannot reach, instantly reducing transepidermal water loss (TEWL) and calming the heat-stressed barrier.
In high-UV months, aggressive chemical peels can increase the risk of Post-Inflammatory Hyperpigmentation (PIH). Our dermatologists utilise Mandelic Acid specifically for its unique molecular structure.
The Mechanism: Mandelic Acid has a significantly larger molecular weight compared to Glycolic Acid. This means it penetrates the skin more slowly and evenly, preventing the “hot spots” or acid burns that can occur when the skin barrier is sensitized by heat.
The Lipophilic Advantage: Mandelic acid is oil-soluble. In a high-humidity climate where sebum production is at its peak, this acid dives deep into the lipid-heavy environment of the pore to break down the debris that causes “Summer Congestion.”
Clinical Benefit: It provides a brightening effect and anti-bacterial action without the downtime or sun sensitivity associated with deeper peels.
For patients with significant Sebaceous Hyperplasia or persistent “midday shine,” the Carbon Laser Peel (also known as the “China Doll” or Q-Switched Peel) offers a long-term thermal solution.
The Mechanism: A medical-grade liquid carbon layer is applied to the face, which acts as a “magnet” for oil and contaminants deep within the pores. As the Q-Switched Nd: YAG laser passes over the skin, the carbon particles implode.
The Thermal Effect: The laser energy destroys the carbon and the debris it has absorbed. More importantly, the thermal energy reaches the sebaceous glands, temporarily shrinking them and reducing their oil-secretion capacity.
Clinical Benefit: It effectively “vacuums” the pores while stimulating collagen. It is an ideal intervention for the summer skincare routine for humidity as it addresses both the oiliness and the large pore size that humidity exacerbates.
The effectiveness of your summer skincare routine for humidity depends on the transition from heavy oils to aqueous, humectant-based layering. By understanding the biophysical changes your skin undergoes in the Kolkata heat, you can prevent the cycle of congestion and inflammation before May arrives.
A generic approach can often exacerbate underlying conditions. For a customised summer skincare routine for humidity based on your specific skin type and sebum levels, we recommend a clinical evaluation.
No, provided the “flooding” is done with non-comedogenic humectants. It is the use of heavy oils, not water, that causes breakouts.
Yes, but with caution. Heat can increase sensitivity. Use a lower concentration or a “sandwich” technique with your water-gel moisturizer.
Dullness is often caused by oxidized oil and sweat. Regular keratolytic cleansing and antioxidant (Vitamin C) application can restore luminosity.

What Are Acne Scars and Why Do They Form?
What Is Fractional CO₂ Laser Treatment?
How Fractional CO₂ Laser Works on Acne Scars
How Fractional CO₂ Laser Helps Fade Acne Scars
Key Benefits of Fractional CO₂ Laser
The Fractional CO₂ Laser Treatment Process
Fractional CO₂ Laser Treatment Cost in India
Who Should Consider Fractional CO₂ Laser?
Possible Side Effects and Aftercare Tips
You know that sinking feeling when you catch your reflection under harsh light — and instead of smooth skin, all you can see are tiny craters and uneven marks left behind by old breakouts.
It feels unfair. You fought acne once, and somehow, you’re still fighting its ghost.
Acne scars don’t just linger on your skin; they quietly mess with your confidence, makeup routines, selfies, and sometimes even your mood. You start wondering if your skin will ever look like it used to.
Here’s the good news: it can.
Fractional CO₂ laser technology has become one of the most effective, dermatologist-preferred solutions for treating stubborn acne scars that refuse to fade with creams or peels. By working deep within the skin, it helps remodel damaged tissue and rebuild smoother, clearer skin from within.
At Wizderm, treatments are performed using the Lumenis UltraPulse CO₂ Laser, a globally trusted medical-grade platform known for its precision, safety controls, and proven clinical outcomes.
In this guide, you’ll learn how fractional CO₂ laser treatment works, why it’s different from older lasers, what results you can realistically expect, and why dermatologists worldwide rely on it for acne scar correction.
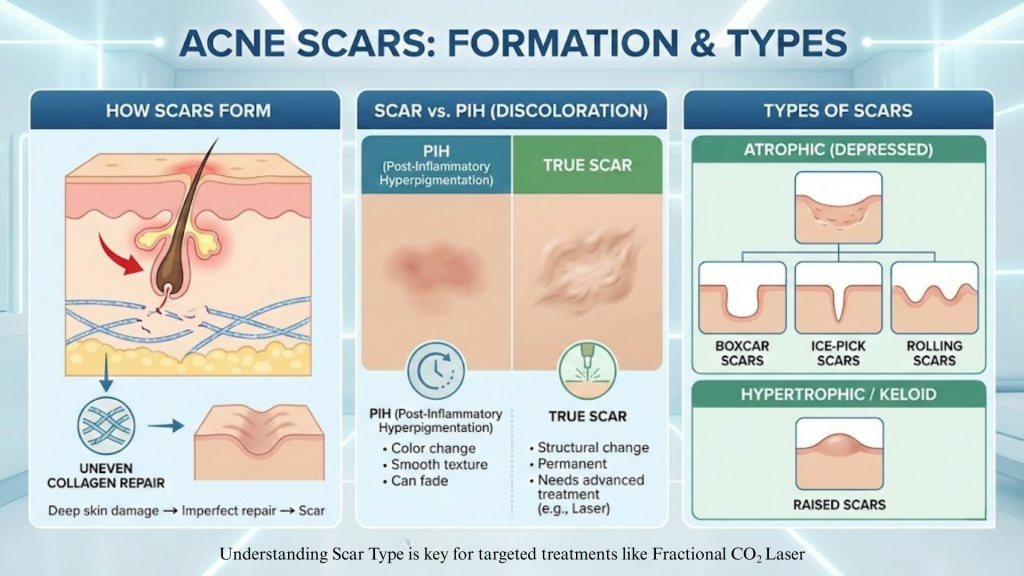
When acne damages the deeper layers of your skin, your body tries to repair the injury by producing collagen. But when this repair process is uneven or insufficient, scars form.
Sometimes what looks like a scar is actually post-inflammatory hyperpigmentation (PIH) — a colour change without texture damage. PIH can fade over time or with topical treatments. True acne scars, however, involve permanent structural changes and require advanced procedures like laser resurfacing.
Understanding your scar type is essential, because fractional CO₂ laser for acne scars works best for certain scar patterns and may be combined with other treatments for optimal results.
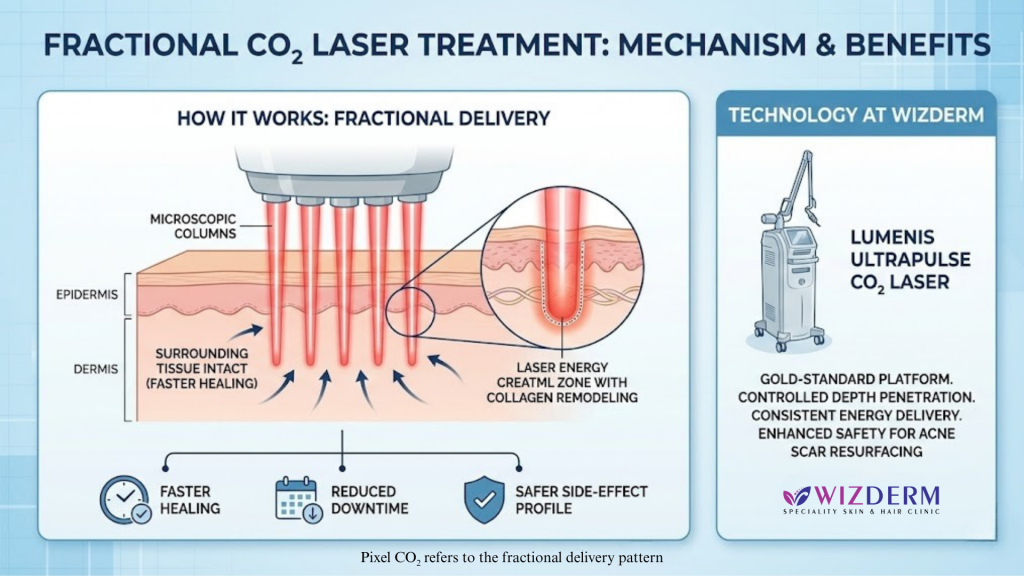
Fractional CO₂ laser treatment is an advanced skin-resurfacing procedure that delivers carbon dioxide laser energy into the skin in thousands of microscopic columns.
Instead of treating the entire skin surface at once, the laser targets only fractions of the skin, leaving surrounding tissue intact. This allows faster healing, reduced downtime, and a safer side-effect profile compared to traditional ablative lasers.
Pixel CO₂ refers to the fractional delivery pattern, not a different treatment altogether. What truly influences your results is the technology and precision of the CO₂ fractional laser machine, combined with the dermatologist’s expertise.
At Wizderm, treatments are performed using the Lumenis UltraPulse CO₂ Laser, a gold-standard platform widely used in dermatology for controlled depth penetration, consistent energy delivery, and enhanced safety — especially important for acne scar resurfacing.
If you’ve ever wished for a “reset” button for your skin, Fractional CO₂ Laser comes close.
The laser creates controlled micro-injuries that stimulate your body’s natural wound-healing response. These microthermal zones activate fibroblasts to produce new collagen and elastin — the building blocks of smooth, firm skin.
This is precisely why fractional CO₂ laser benefits go beyond surface improvement. Over time, depressed scars lift, texture evens out, and skin quality improves from within.
Many dermatologists prefer fractional technology because it balances visible results with a safer recovery profile.
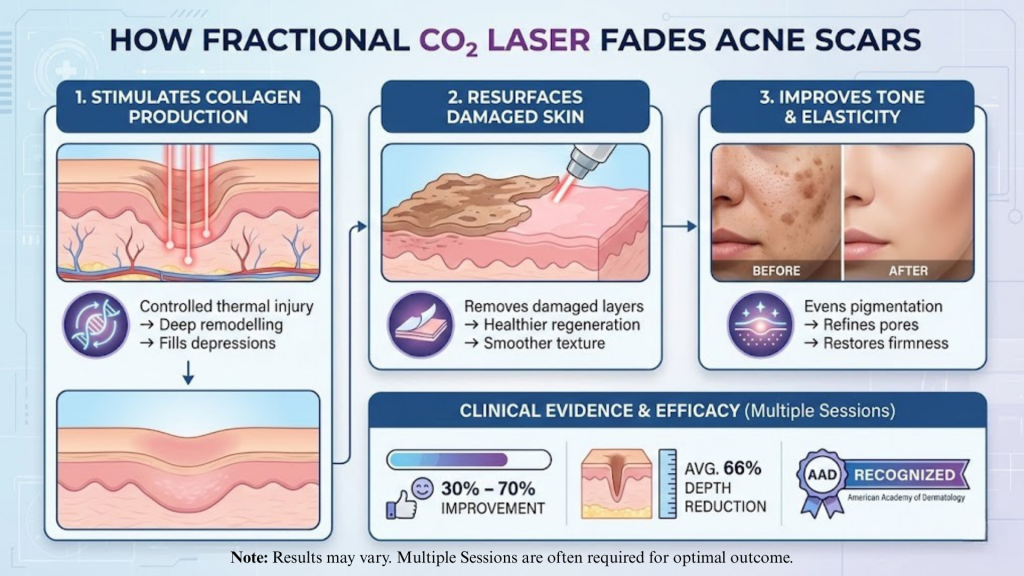
1. Stimulates Collagen Production
Controlled thermal injury promotes deep collagen remodelling, gradually filling in depressed scars and improving firmness.
2. Resurfaces Damaged Skin Layers
Damaged superficial layers are removed, allowing new, healthier skin to regenerate with smoother texture.
3. Improves Tone and Elasticity
Beyond scars, the treatment can help even out mild pigmentation, refine pores, and restore overall skin quality.
Clinical studies indexed on PubMed and National Center for Biotechnology Information report 30%–70% improvement in acne scar appearance, with topographic depth reductions averaging around 66% after multiple sessions.
The American Academy of Dermatology recognises laser resurfacing as an effective option for acne scars when topical treatments are insufficient.
Many patients also notice brighter skin, refined pores, and an overall improvement in skin quality.
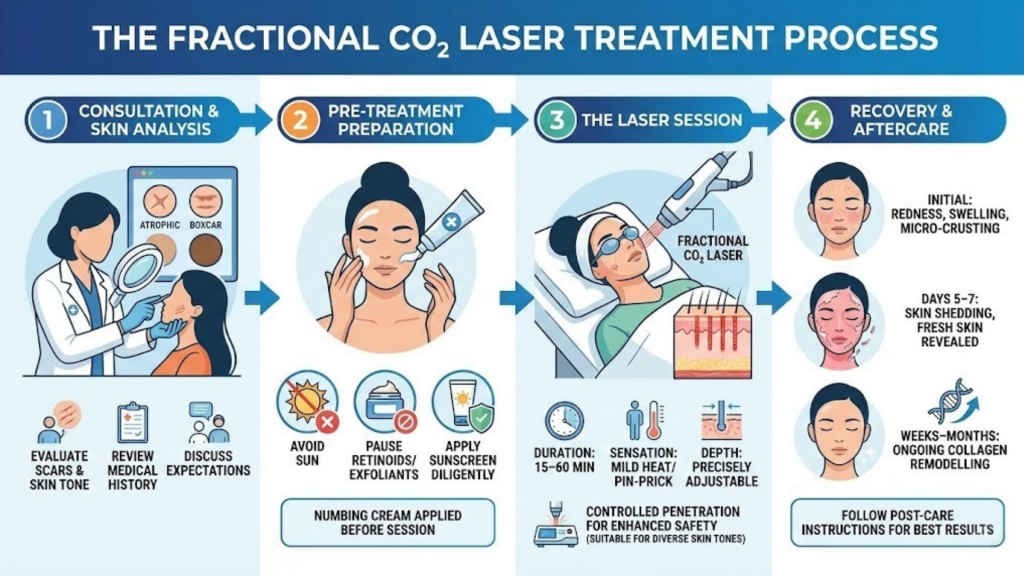
Step 1: Consultation and Skin Analysis
Your dermatologist evaluates scar types, severity, skin tone, medical history, and expectations.
Step 2: Pre-Treatment Preparation
You may be advised to pause retinoids or exfoliants, avoid sun exposure, and apply sunscreen diligently. Numbing cream is applied before treatment.
Step 3: The Laser Session
Advanced fractional CO₂ laser treatment protocols using platforms like UltraPulse allow controlled penetration, improving safety even for Indian skin tones when handled correctly.
Step 4: Recovery and Aftercare
Redness, swelling, and micro-crusting are expected initially. Skin typically sheds by days 5–7, revealing fresh new skin. Collagen remodelling continues for weeks to months.
Most people need 3–4 sessions spaced several weeks apart. While improvement can be dramatic, complete scar removal is rare — especially for deep ice-pick scars.
The fractional CO₂ laser cost in India generally ranges from ₹3,000 to ₹15,000+ per session, depending on the clinic, city, and treatment area.
For small areas or mild scarring, costs are usually on the lower end. Full-face fractional CO₂ laser treatment or deeper acne scars require higher energy settings and may cost more per session.
Because acne scars often need multiple sessions, the fractional CO₂ laser treatment cost for a complete series typically ranges between ₹20,000 to ₹50,000, depending on:
While cost is an important factor, choosing a clinic based solely on price can increase the risk of complications. With laser treatments, precision, experience, and post-care protocols matter far more than discounts.
a. Ideal Candidates
b. Who Should Use Caution
A dermatologist consultation is essential before treatment.
Temporary side effects may include redness, swelling, sensitivity, peeling, or post-inflammatory hyperpigmentation. These usually resolve with proper aftercare.
Aftercare essentials:
Peels, microneedling, creams — most acne scar treatments only skim the surface. The Pixel CO2 Laser goes deeper, using smart fractional technology to stimulate collagen and resurface skin from within.
Unlike traditional lasers, it targets only micro-zones of skin, promoting faster healing and smoother, firmer results.
At Wizderm, our dermatologists tailor every Pixel CO2 Laser session to your unique skin type and scar pattern. Whether your concern is pitted acne scars, uneven tone, or dull texture, the treatment plan is customised for maximum results with minimal downtime.
And the results speak for themselves: smoother texture, refined pores, and clearer, more confident skin that doesn’t need filters.
Acne scars don’t have to define your skin forever. With fractional CO₂ laser treatment, you have a scientifically supported option that targets scars at their core — not just the surface.
If you’re searching for fractional CO₂ laser treatment near me, choosing the right technology and dermatologist makes all the difference.
At Wizderm, treatments are performed using the Lumenis UltraPulse CO₂ Laser and personalised protocols tailored to your scar type and skin tone.
Book your consultation today and take the first step toward smoother, more confident skin.
Most people require 3–6 sessions depending on scar depth and skin response.
Discomfort is minimal with numbing cream; most patients describe mild heat or tingling.
Initial healing takes about 5–7 days, with continued improvement over months.
Yes, fractional CO₂ laser can be safe for Indian skin tones when performed by experienced dermatologists using appropriate settings and strict aftercare

You’re Over-Cleansing and Destroying Your Skin Barrier
You’re Stuck in the Micro-Trauma Cycle
Your Haircare Is Secretly Causing Your Forehead Acne
Your Gut and Skin Are in a Fight (And Your Skin Is Losing)
Cortisol (Stress Hormone) Is Sabotaging Your Skin
The Things Touching Your Face Are Dirty (Even If Your Skin Isn’t)
Bonus Reason: You’re Product-Hopping Too Fast
Isn’t it painfully ironic that acne loves showing up right before an important presentation, a wedding function, or a first date?
If pimples were polite, dermatology clinics wouldn’t exist.
You’ve likely tried multiple cleansers, serums, spot treatments, and DIY fixes. Your shelf is crowded. Your wallet is lighter. Your acne? Still very much present.
Here’s the uncomfortable truth most people miss:
Acne doesn’t persist because you’re not doing enough — it persists because you’re doing the wrong things consistently.
At Wizderm, we see this pattern daily. Patients aren’t careless. They’re misinformed.
Let’s fix that.
The idea that “clean skin = acne-free skin” sounds logical — and is completely wrong.
Your skin has a protective barrier made of lipids, oils, and beneficial bacteria. This barrier:
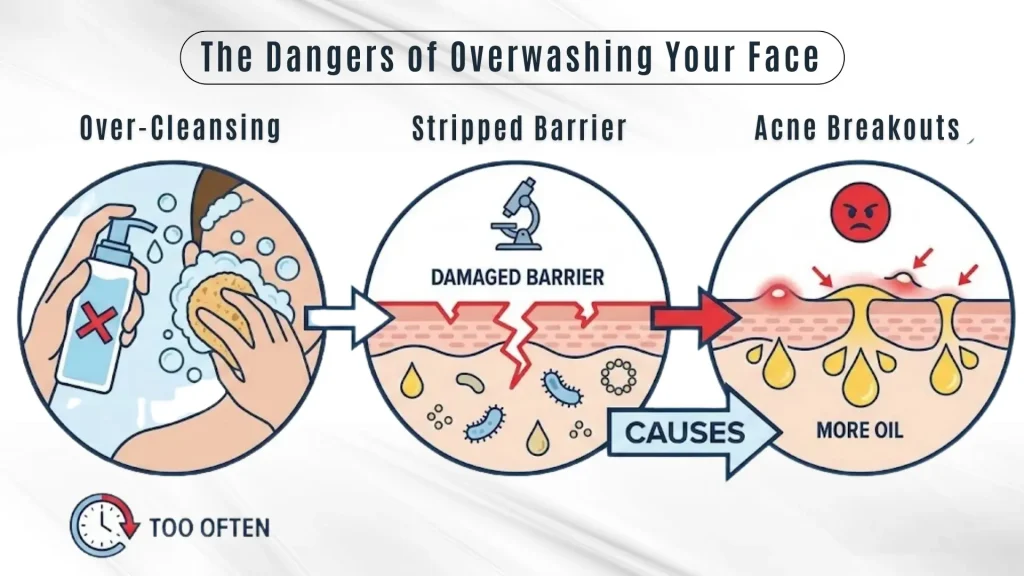
When you wash your face too often or use harsh foaming cleansers, you strip this barrier. Your skin panics and responds by producing even more oil, which clogs pores and fuels breakouts.
“A compromised skin barrier is one of the most overlooked causes of persistent acne. Patients often worsen their acne by over-cleansing rather than under-cleansing.”
— Consultant at Wizderm Skin & Hair Clinic
Pro tip: If your skin feels “squeaky clean” or tight, that’s damage—not cleanliness.
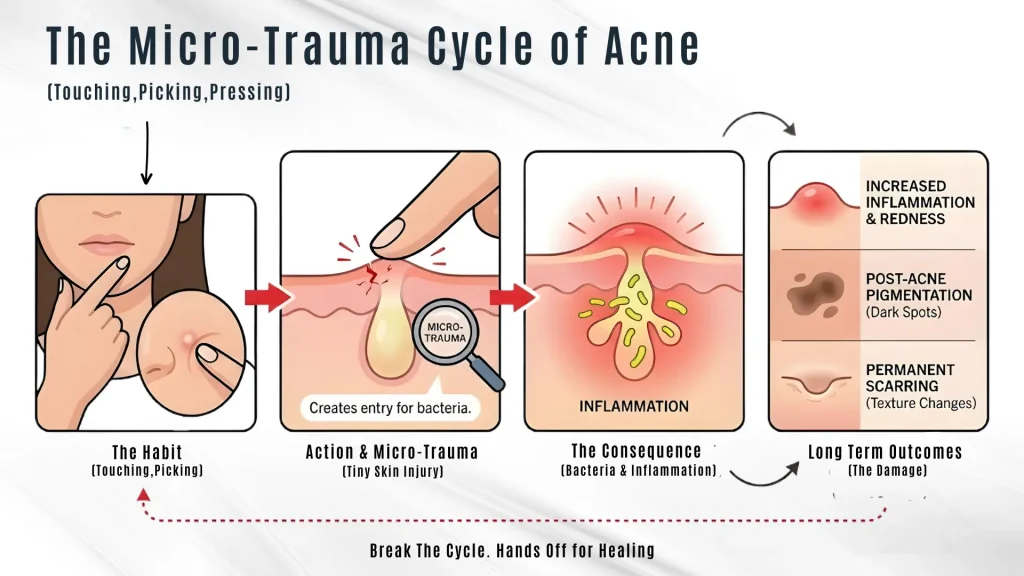
We all do it. Resting your chin on your hand. Touching a bump. Picking “just a little.”
Each time you touch your face, you create “micro-traumas”—tiny skin injuries that invite bacteria and inflammation.
Studies show people touch their face 20+ times per hour. That’s acne fuel on autopilot.
Squeezing pimples doesn’t “empty” them. It pushes bacteria deeper, increasing:
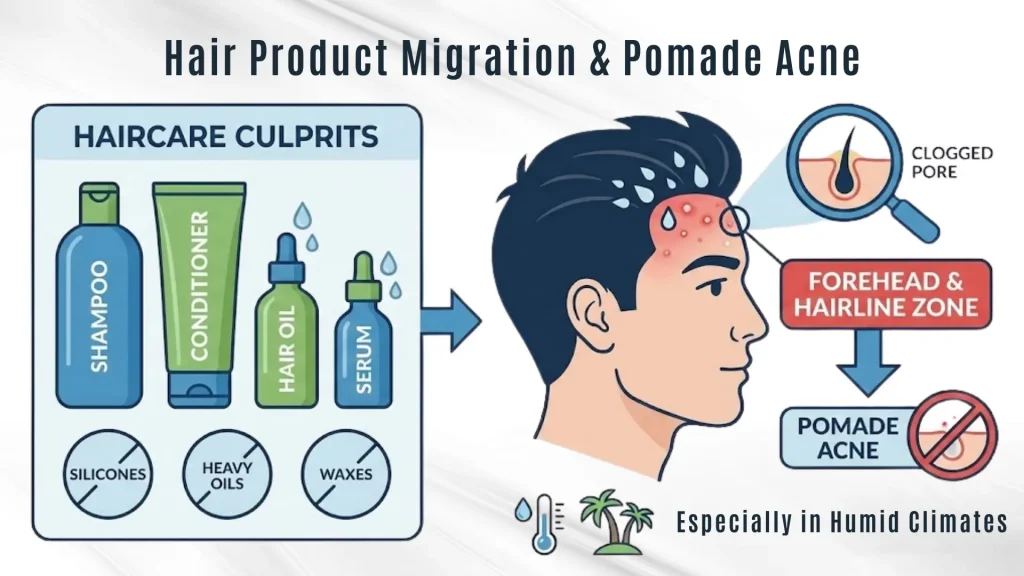
If your breakouts sit around the forehead, temples, or hairline, your skincare may be innocent — your hair products are not.
Shampoos, conditioners, serums, and oils often contain:
These migrate onto facial skin, clog pores, and cause pomade acne, especially in humid climates like India.
Dead giveaway: Acne that follows the exact line of your bangs, helmet strap, or dupatta edge.
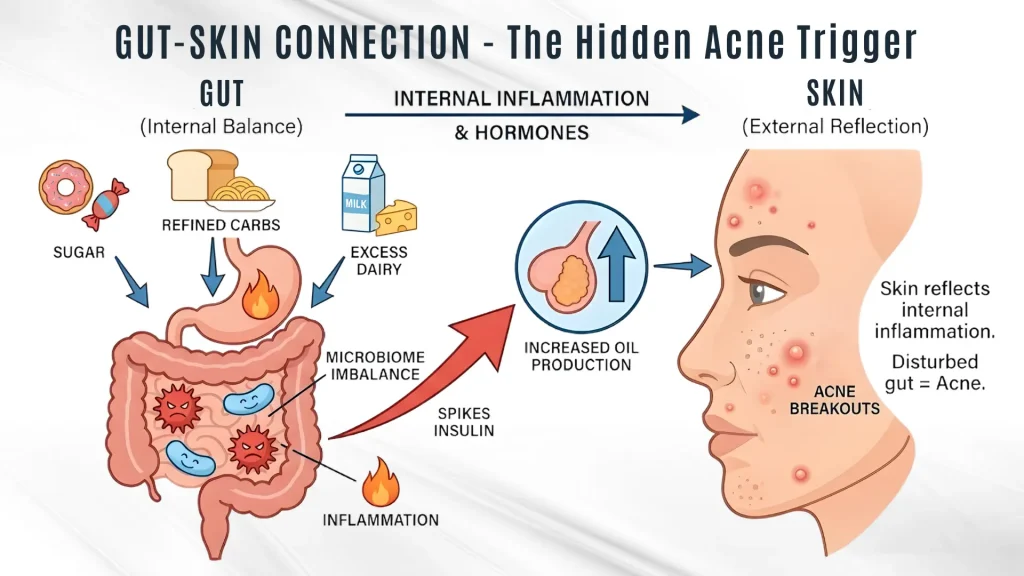
Your skin reflects internal inflammation. Period.
Diets high in:
Spike insulin levels, triggering hormones that increase oil production and acne.
Emerging research in Dermatology Reports shows the gut microbiome plays a major role in controlling skin inflammation. When gut balance is disturbed, acne often follows.
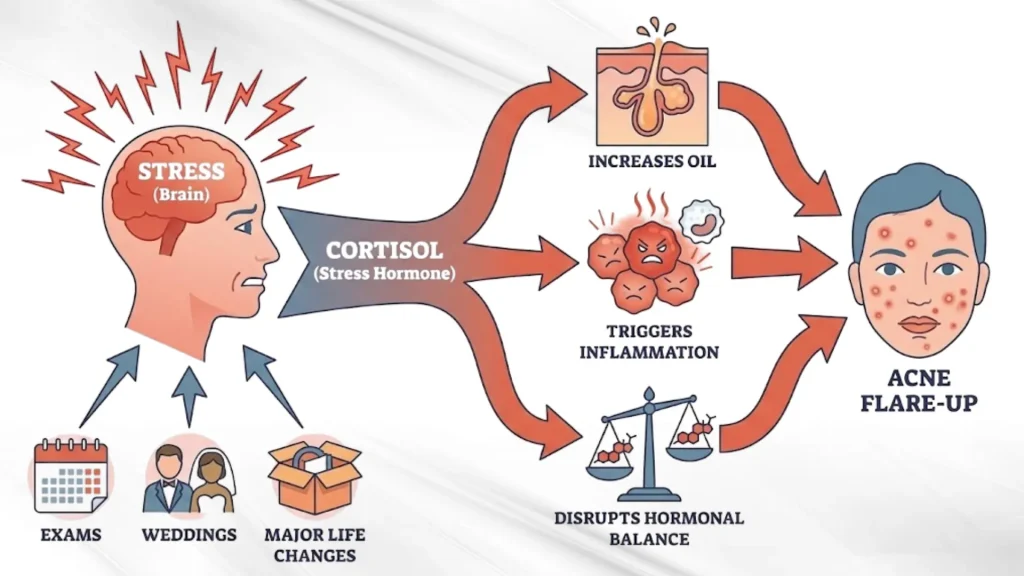
Stress doesn’t just live in your head — it shows up on your face.
When you’re stressed, cortisol:
This explains why acne flares before exams, weddings, or major life changes.
If your acne worsens during stressful phases, a dermatologist can help break the stress–acne cycle clinically.
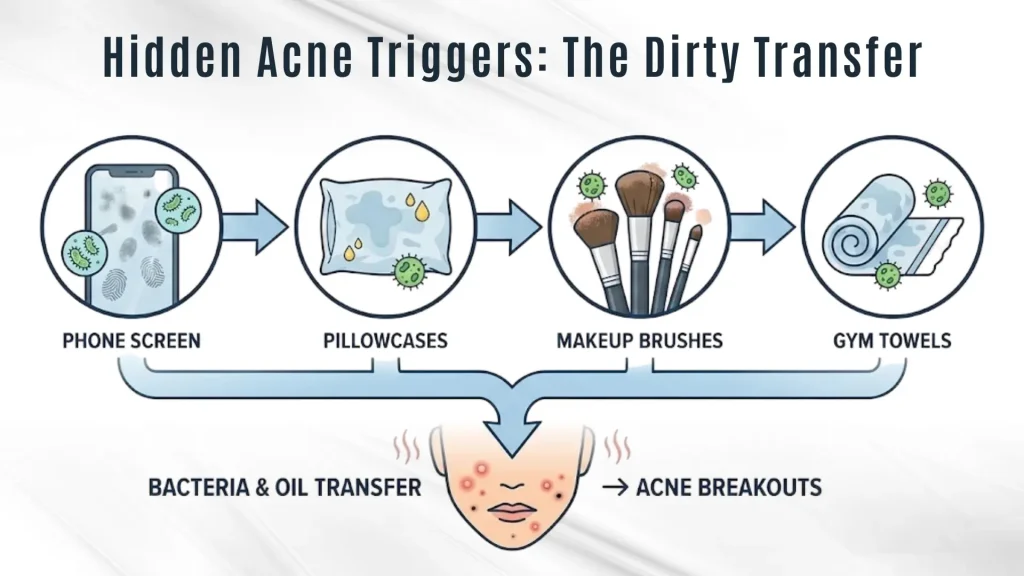
Your phone screen. Pillowcases. Makeup brushes. Gym towels.
They collect oil, sweat, and bacteria — and transfer them straight onto your pores.
Studies from Northwestern Medicine show mobile phones carry more bacteria than toilet seats. Combine that with facial heat, and breakouts thrive.
Small hygiene upgrades = big acne improvements.
Acne treatments don’t work overnight.
Constantly switching products:
Most acne treatments need 6–8 weeks to show results. Mild purging is normal. Chaos is not.
Cleanser → Treatment → Moisturiser → Sunscreen (AM only)
If acne worsens or burns, stop experimenting and see a professional.

If your acne:
…it’s time to stop DIY-ing.
At Wizderm, dermatologists identify the root cause — hormonal, bacterial, inflammatory, or lifestyle-related — and create personalised treatment plans, including:
Acne is rarely just a skin problem. It’s a reflection of your habits, hormones, stress, and skin barrier working (or not) together.
The good news? Acne is treatable and manageable with the right approach.
At Wizderm, we combine science-backed dermatology with personalised care, so you’re not just treating pimples — you’re preventing them long-term.
👉 Book your consultation today and take the first real step toward clearer skin.
Recurring acne often means the root cause hasn’t been addressed. Hormones, stress, skincare mistakes, or incomplete treatment can all lead to relapses.
Stress, hormonal imbalances, lifestyle changes, and disrupted sleep cycles make adult acne increasingly common, especially in women.
Acne can’t always be “cured,” but with consistent dermatological care, it can be controlled long-term and prevented from recurring.
Most treatments show visible improvement in 6–8 weeks, with continued improvement over 3–6 months.
While complete removal is rare, advanced treatments like lasers and microneedling can dramatically reduce scars and improve skin texture.
In this Article

Breakouts are frustrating, but it’s the post-acne aftermath that truly lingers. Even after the pimples fade, you may still be dealing with uneven texture, dark marks, and the bigger question: what actually works for acne scar removal?
While makeup and filters offer a quick cover-up, dermatology offers something better: clinically proven acne scar treatments that rebuild the skin where scars form. With the right diagnosis and a personalised plan, smoother, more confident skin is absolutely possible. Let’s take a closer look at how.
Ever tried unlocking a lock without knowing which key fits? That is exactly what happens when you try treatments for removing acne scars without knowing what kind of acne scar you are dealing with. Dermatologists know that accurate diagnosis is half the cure, because how to treat acne scars depends entirely on the types of scars you have.
Here’s the breakdown of the most common types of acne scars, and how each one responds to specific treatments.
Ice pick scars are deep, narrow, V-shaped scars that seem like someone poked your skin with a needle. It is caused by severe cystic acne that destroys collagen and leaves behind pits.
These are the toughest to treat and rarely respond to topical acne scar treatment products alone. You’ll likely need in-clinic interventions for visible improvement
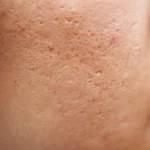
Boxcar scars are broad, U-shaped scars with sharply defined edges, creating a pitted look. These are caused by inflammatory acne that damages collagen, leaving behind shallow to moderate depressions on the skin.
These scars are commonly found on the cheeks and temples, and often become noticeable under certain lighting.
These kinds of acne scars can be treated with fractional lasers, microneedling, and dermal fillers to improve their depth and overall appearance.

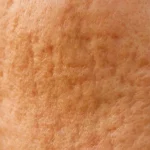
Rolling scars look like wide, shallow depressions with smooth, wave-like edges; think of them as gentle dips across the skin. These scars occur due to damage to subcutaneous tissue that creates fibrous bands pulling down the skin.
These are treated with the help of subcision to release the tethered skin, Microneedling, a combination of laser resurfacing, and acne scar treatment at home.
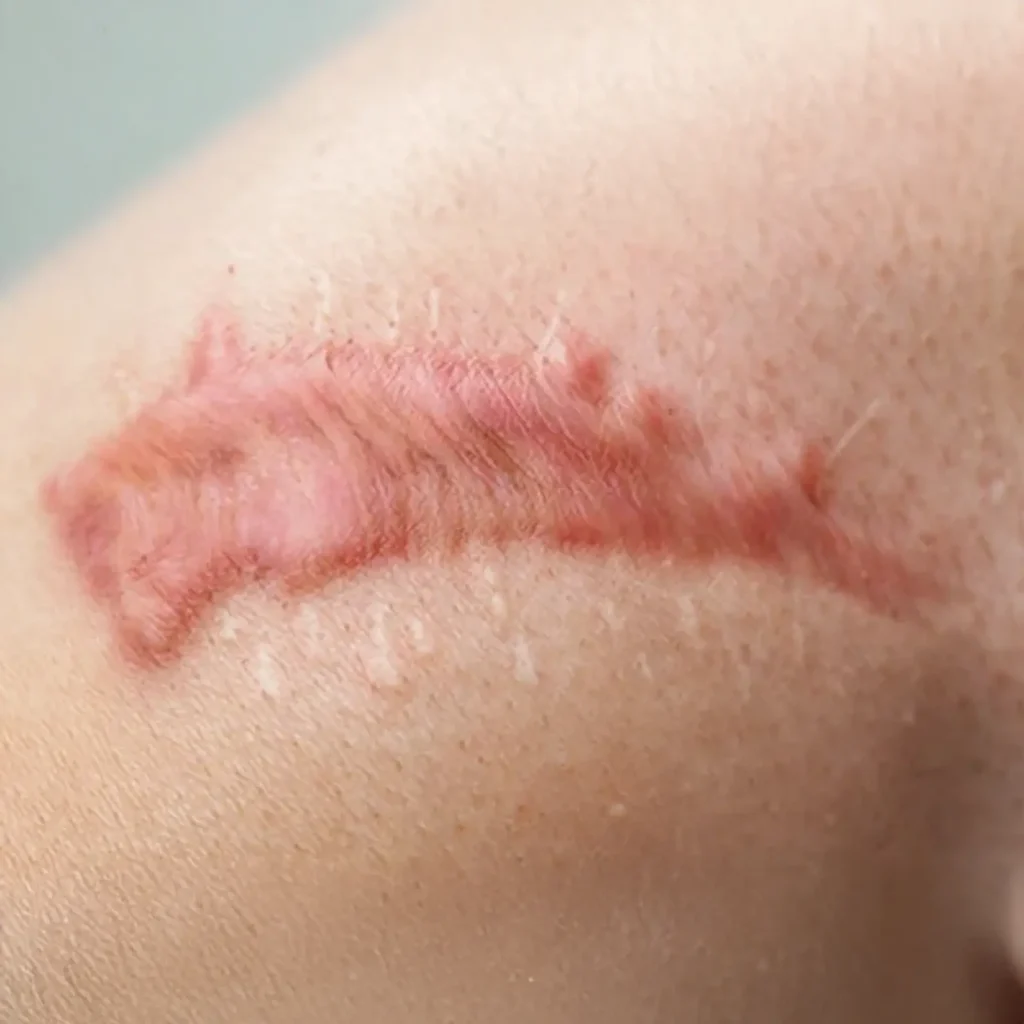
Hypertrophic and keloid scars are raised, thick, rubbery areas of scar tissue that form when the skin produces too much collagen during healing.
Unlike hypertrophic scars, which stay within the original wound boundary, keloids can grow beyond the initial acne lesion and continue expanding over time.
They may appear pink, red, or deep brown, and can feel firm, itchy, or even tender. These scars are more common in darker skin tones, those with a family history of keloids, and individuals prone to inflammatory ac
When we say “dermatologically approved,” we’re not tossing around fancy jargon. What it really means is this: the treatments you use are clinically backed, tested for safety, and designed to create real change, not temporary brightness or optical tricks that fade in a few days.
If you’ve been struggling with acne scars, here’s what truly dermatology-approved care means for you:
Dermatologists don’t rely on trends; they rely on evidence. Whether it’s laser skin resurfacing or prescription topicals, every recommendation is rooted in clinical research.
For example, fractional CO₂ laser treatments can reduce atrophic acne scars by 60–80% in just 3–5 sessions. That’s not an estimation; it is a documented, repeatable improvement.
On the topical side, your dermatologist may recommend proven actives like:
And if you’re using acne scar removal creams or face washes, they’ll ensure the actives are in the right concentration and formulation so you get real results, not irritation.
There’s no universal fix for acne scars. That’s why dermatology always starts with your skin.
Depending on your scar type, your plan may look different:
Your skin tone also influences your treatment path. For deeper skin tones, certain lasers can be risky, so dermatologists may choose safer options like Radiofrequency with Microneedling (MNRF), effective but gentler
Dermatologically approved means no DIY acid peels, no unregulated serums.
Every step, from the strength of a chemical peel to the depth of microneedling, is controlled by trained experts who understand your skin barrier, healing time, and long-term safety.
You get treatments that work without compromising your skin.
You’re never left alone to “figure it out.” Dermatologists adjust your plan as your skin changes. You might follow a blended routine, clinic sessions plus a simple at-home regimen, to steadily improve your scars.
Your progress is tracked. Your reactions are monitored. Your results are protected.
When it comes to acne scar removal, in-clinic treatments aren’t just effective—they’re elite. Think of them as the haute couture of scar repair: tailored, high-performance, and backed by dermatological science. These aren’t your DIY scrubs or over-the-counter wishful thinking—these are the gold standard solutions prescribed by skin experts who know their lasers from their lotions.
Here’s what’s dominating the dermatologist offices in 2025 and why they’re worth every session
Laser Skin Resurfacing is a cornerstone of professional acne scar treatment, offering targeted precision to reduce scar depth and improve overall skin texture. By stimulating collagen production, lasers help remodel damaged skin and restore a smoother, more uniform surface.
The types of lasers used for acne scars can vary depending on the type of scars:
Each laser resurfacing session typically costs around Rs 7,000 to Rs 12,000 per session. You will need 3 – 6 sessions across 6 months, depending upon your scar type and intensity, with a downtime of 3-7 days.
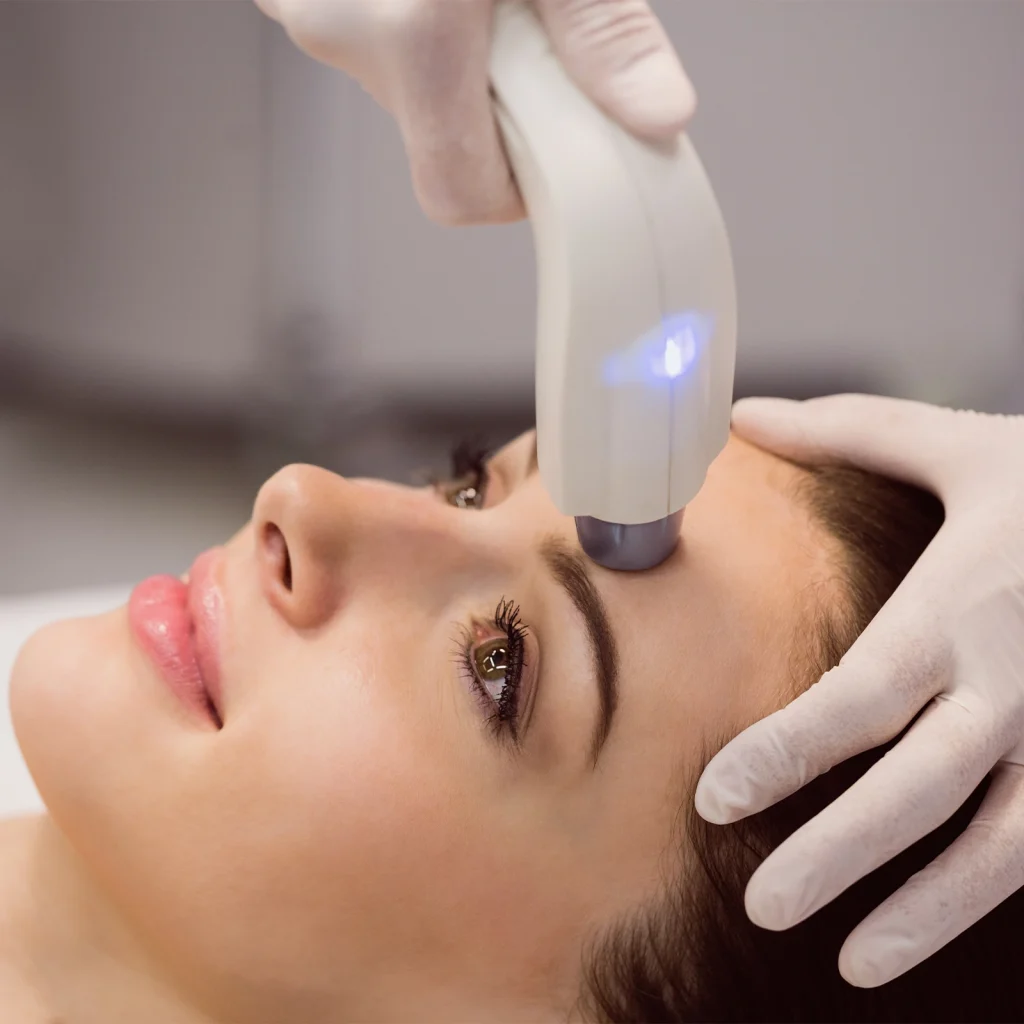
Microneedling, also known as collagen induction therapy, utilises fine needles to create controlled micro-injuries, thereby triggering the skin’s natural healing process. When combined with Platelet-Rich Plasma (PRP), the treatment becomes even more effective due to the regenerative growth factors in your plasma.These are best suited for rolling scars, mild boxcar scars, and uneven skin texture.
At Wizderm, you will find an innovative approach to microneedling. We add microneedling with radiofrequency (MNRF).
The treatment can cost you between Rs 5000 – Rs 25000, depending upon the severity, with a downtime of 1-3 days.
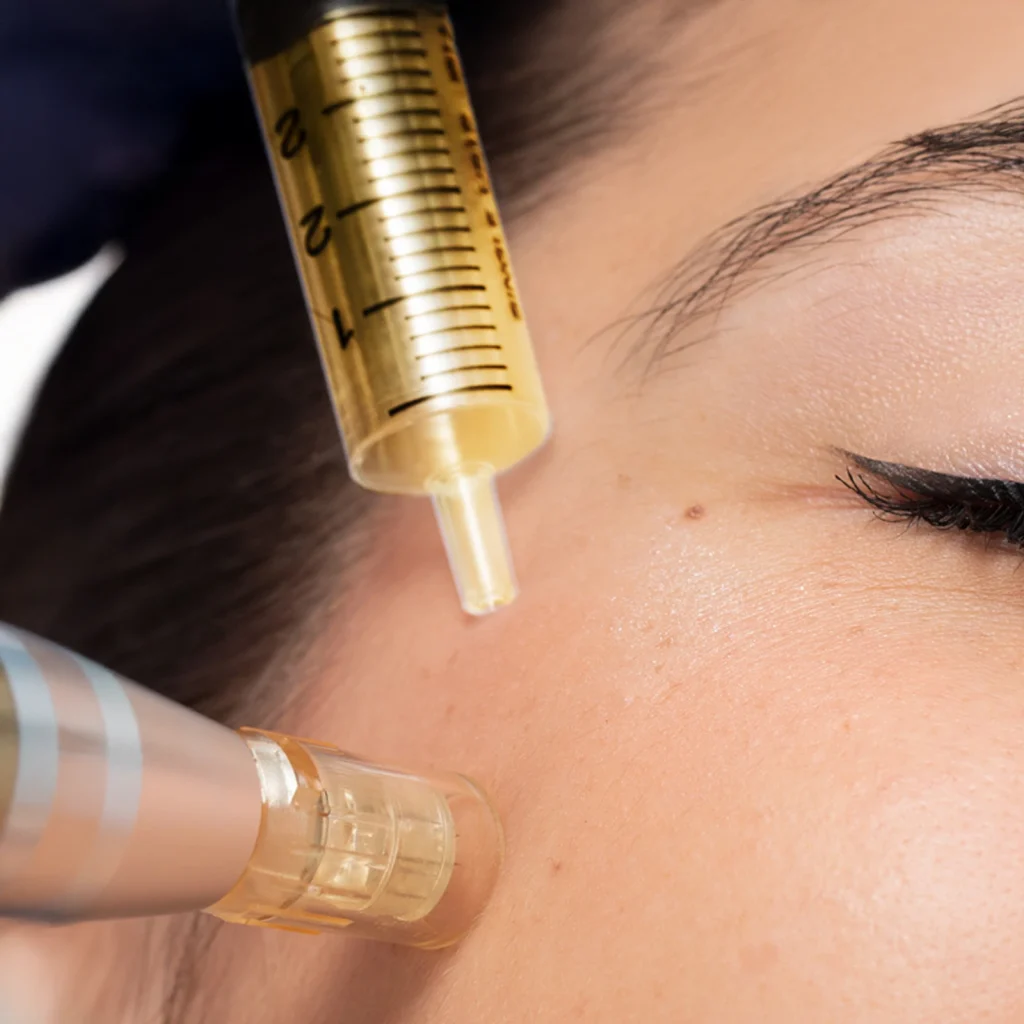
Professional-grade Chemical Peels use controlled exfoliation to remove damaged skin layers, reduce pigmentation, and refine texture. Dermatologists customise peel strength and frequency based on individual skin types and scar severity. This treatment is best suited for superficial scarring.
The downtime for this procedure is extremely minimal, say, 1-7 days and does not put a hole in your pocket as each session can range between Rs 1,500– Rs 5,000.

Subcision is a minor surgical technique that breaks down fibrotic tissue, pulling the skin down. This releases tethered scars and allows the skin to rise and smooth out over time. These are indicated for: Rolling scars and select boxcar scars.
Subcision has shown 60–70% improvement with just 1–2 sessions, especially when followed by fillers or laser treatments. Downtime is minimal, like mild swelling for 2-3 days, and results are often long-lasting.
Each session can cost you between Rs 6,000–Rs 15,000 per session.
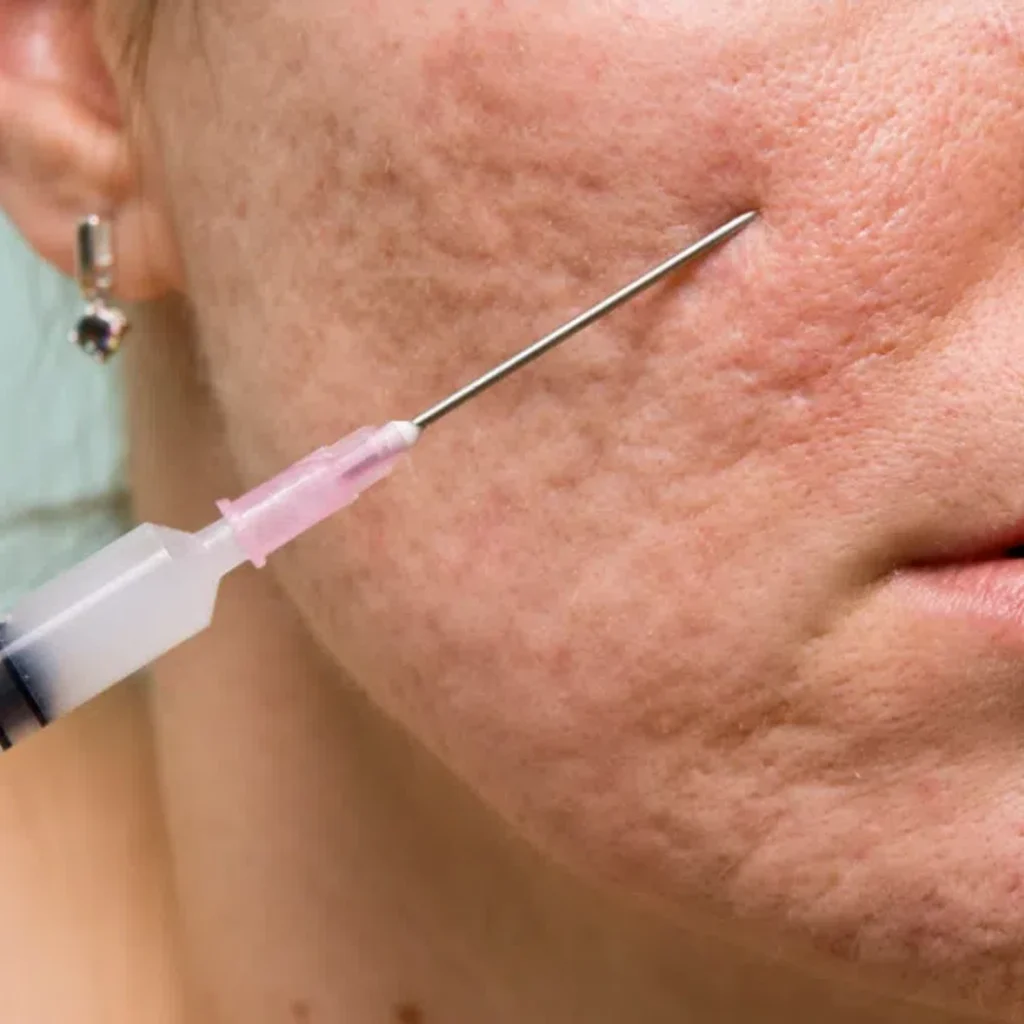
Dermal Fillers like hyaluronic acid are injected under indented scars to “lift” them up, providing an immediate improvement in skin texture. Though not permanent, they’re a fantastic bridge while waiting for collagen-boosting treatments to kick in.
Fillers can stay on for 12-18 months and can range between Rs 15000- Rs 25000, depending upon the scarring.
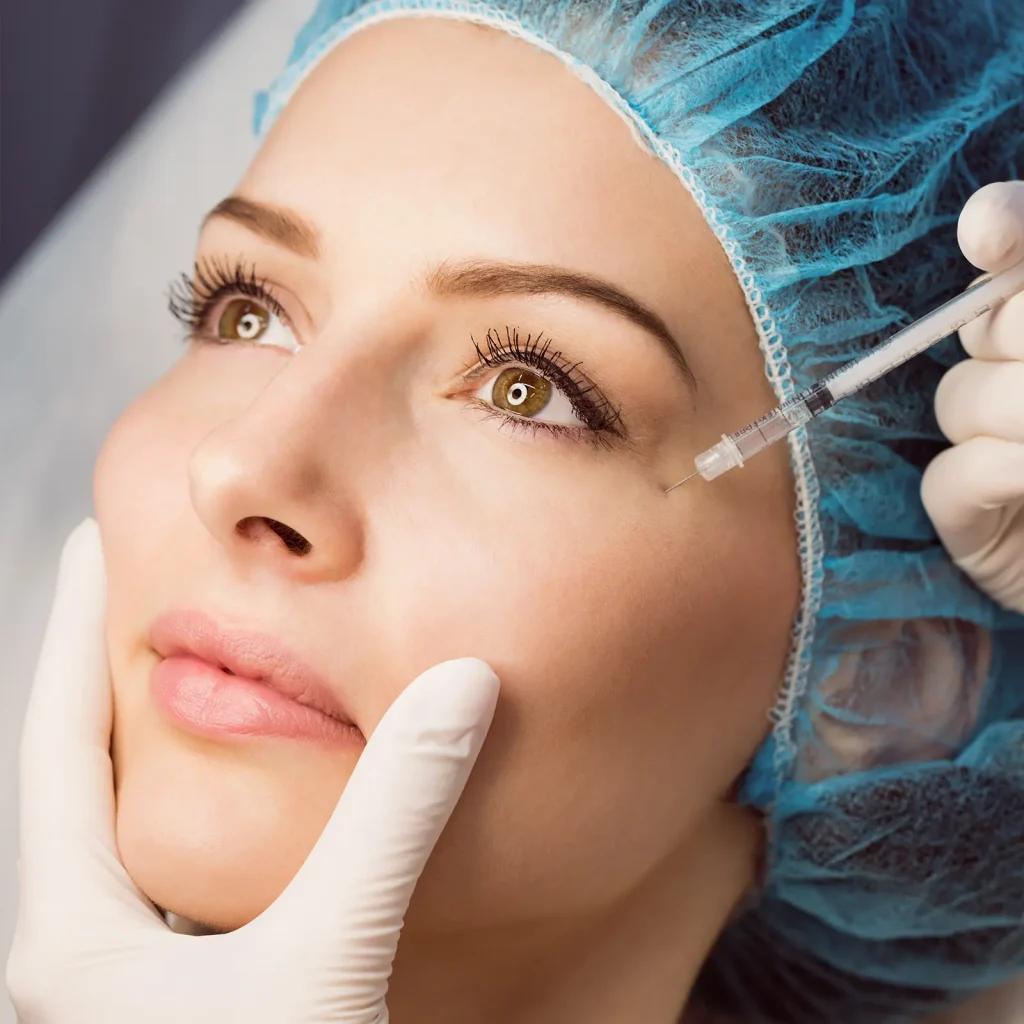
This precise chemical technique uses high-strength trichloroacetic acid to target individual ice pick scars, triggering controlled inflammation and collagen regeneration. This treatment is best suited for deep, narrow scars that don’t respond to lasers or peels.
This procedure can range between Rs 3000 – Rs 8000 per session.

If you’re not clinic-bound just yet, good news: acne scar treatment at home can be effective, if done right and consistently.
These include:
Topical treatments typically show visible improvements within 8 to 12 weeks. Microneedling and PRP therapies may take around 3 to 6 months to deliver full results.
Fillers offer immediate results, though the effects are temporary. The common thread across all these options? Consistency.
A 2023 study published in Dermatologic Surgery found that patients who followed a combined 6-month regimen involving lasers, chemical peels, and at-home retinoids reported an impressive 80–90% satisfaction rate with their scar reduction outcomes.
Here’s the truth: complete acne scar removal is rare. But “barely noticeable” is very possible.
Scars are, by nature, permanent changes in the skin’s structure. However, with derm-grade interventions, most people achieve:
Expect scars to become visibly minimal and well-blended with your natural skin texture, rather than completely erased like a retouched image.
At Wizderm, we understand that each acne scar needs a different approach. So, every treatment plan is:
We combine:
Our goal is simple: to help you regain smoother, more confident skin, with the safest and most effective dermatological approach.
Acne scars can be stubborn, but science is firmly on your side. With the right diagnosis, consistent care, and dermatologist-led treatment, you can dramatically minimise scar visibility and restore a smoother skin texture.
Whether you’re starting with gentle at-home actives or ready for advanced procedures like lasers or microneedling, improvement is not just possible, it’s proven. Clinical treatments can deliver scar reduction, and a well-structured 6-month plan can take you from self-conscious to skin-confident.
Book a consultation with Wizderm and let’s build a personalised, clinical strategy that helps you finally see and feel the difference.
Yes, acne scar removal treatments can be safe for darker skin tones when performed by experienced dermatologists using the right techniques and technologies. However, it’s crucial to customise treatments—especially lasers and peels—to minimise the risk of post-inflammatory hyperpigmentation.
Acne scars are physical changes like indentations or raised areas, caused by damage from acne. However, dark spots are flat areas of discolouration caused by post-inflammatory hyperpigmentation (PIH), where the skin produces too much melanin after inflammation.
There aren’t any age restrictions regarding acne scar removal treatments, but there are factors to consider, particularly for younger individuals. Effective treatments are available for people of all ages, but the optimal time to treat scars is often when acne is under control and there’s minimal risk of future flare-ups.
Acne marks are unlikely to resurface exactly as they were treated. They may appear to be recurring; new ones may arise if the underlying problem is not treated. Lasers, microneedling, and chemical peels can help to reduce the look of acne; nevertheless, new acne can generate new scars.
Yes, many acne scar treatments—like chemical peels, microneedling, or laser therapy—can temporarily increase your skin’s sensitivity. This happens because these procedures exfoliate or penetrate the skin to stimulate healing. You may experience redness, dryness, or a heightened reaction to sun exposure and skincare products. Always follow post-treatment care instructions and use sunscreen to protect your skin and support its recovery while minimising irritation or sensitivity.
Downtime varies by treatment. Chemical peels may cause redness and peeling for 3–7 days. Microneedling typically has 1–3 days of redness. Laser treatments, especially ablative types, can require 1–2 weeks of healing. Dermal fillers usually have minimal downtime—just slight swelling or bruising. Each skin type responds differently, so always consult a dermatologist for personalised guidance and follow aftercare instructions to speed up recovery and avoid complications.
In this Article
What is hormonal acne? How can you prevent it?
What are the root causes of hormonal acne?
What does hormonal acne look like?
Hormonal acne vs fungal acne: What’s the difference?
How to prevent and control hormonal acne?
Prescription oral treatments and cosmetic procedures
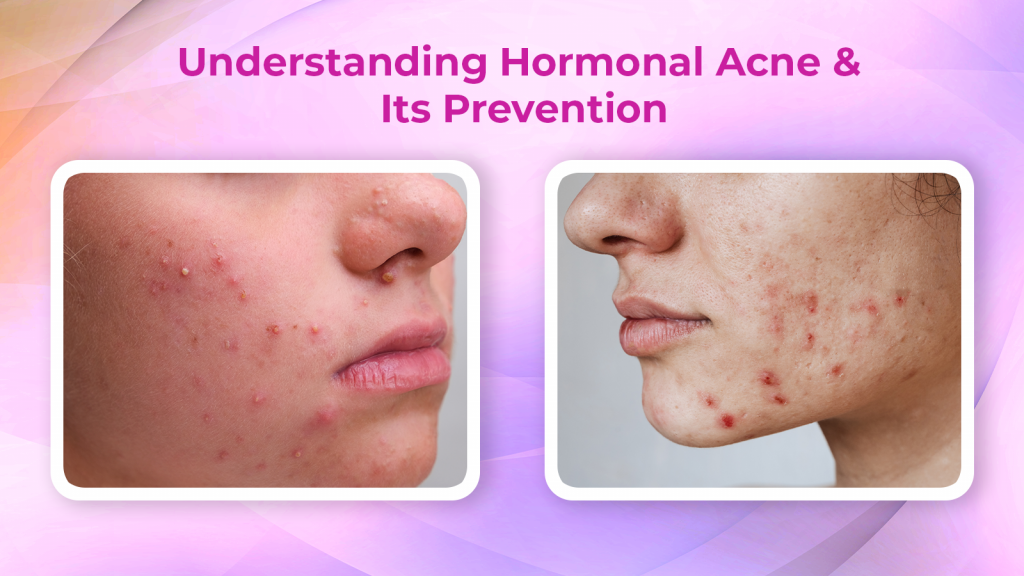
The thought of painful, inflamed and pus-filled acne breakouts can instantly gross somebody out. These enormous-looking pimples are called ‘hormonal acne’, which can result from a combination of reasons like insulin spikes, high cortisol levels, puberty, poor diet, and lack of physical activity.
The major cause of these lesions is hormonal fluctuations. While all of these may sound baffling, this blog emphasises what hormonal acne is, what causes it, and how to prevent it with natural remedies and medical treatments. Read to know more.

Reviewed by Dr. Swarnali Maiti
MBBS, MD in Dermatology, Venerelogy & Leprosy
Updated on: July 5, 2025
Hormonal acne, or commonly known as adult acne, is directly caused by the presence of excess sebaceous (oil) glands, and is commonly found to affect men and women between the ages of 20 and 50. The blockage of pores caused by sebum, dirt or product buildup can cause acne.
Hormonal acne could cause bumps on an individual’s face, chest, shoulders, and back in the form of cysts, pimples, whiteheads and blackheads. It is to be noted that hormonal imbalance acne is more common in women than in men, research showing that approximately 80.9% of women are predominantly affected when compared to the 19.1% of male adult acne patients.
Firstly, it is to be noted that hormonal acne patients experience more breakouts in the following phases:
To understand which hormones play a role in causing acne, researchers surmise that the hormone androgen can be linked to the condition. While androgens are found in both males and females, the concentration is lower in case of women. The presence of excess androgens in women causes the oil glands to produce uncontrollably more sebum than usual, hence, inducing acne flare-ups.
Thereafter, the level of androgen (the hormone that causes acne in females) in the body can increase because of the following factors:
Nonetheless, androgen hormone levels in the body (both men and women) can also increase due to poor dietary choices such as dairy, gluten and sugar.

Hormonal acne symptoms can manifest as painful, deeper papules, pustules, cysts and nodules on one’s lower cheeks, jawline and chin. Some signs can also occur as non-itchy whiteheads and blackheads. These damaged skin tissues or lesions can appear red, be filled with pus and even feel sore just by the thought of touching the affected area.
Besides one’s face, neck, back, chest, and shoulders are other common areas where hormonal acne may occur. Picking at the blemishes or squeezing them can worsen the condition, transferring the germ to other nearby areas.
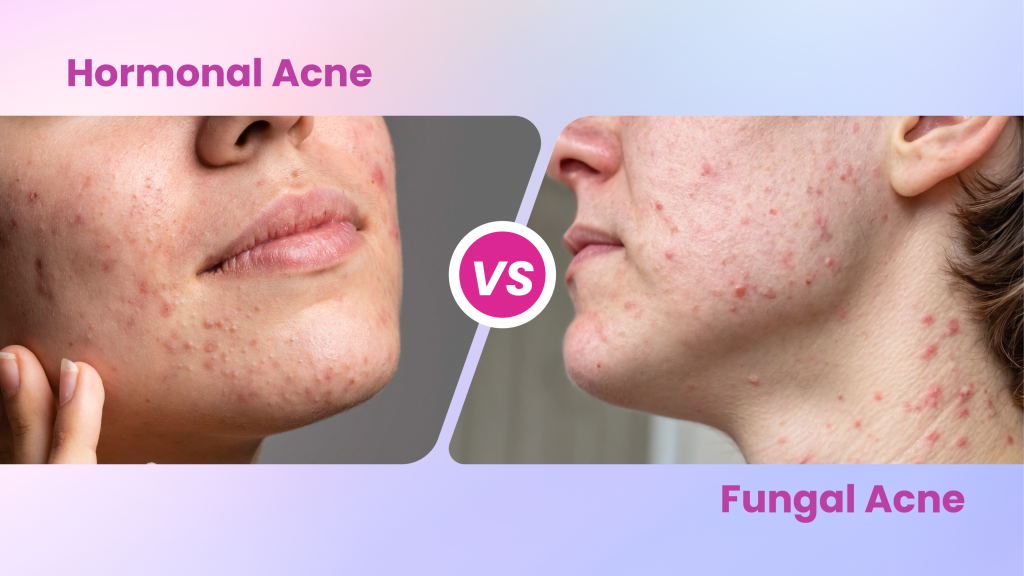
Hormonal imbalance acne may often be mistaken for fungal acne, as both occur in the hair follicles; however, they have distinctive characteristics. Hormonal imbalances lead to the production of excess sebum, hence causing clogged pores and hormonal acne.
On the other hand, the overdevelopment of Malassezia yeast on the skin impacts the hair follicles and results in a cluster of small, often with red borders, uniform, itchy bumps on the forehead, chin, cheeks, upper back, shoulders and chest.
Antifungal treatments are ideal for managing fungal acne, whereas hormonal acne responds well to targeted sebum-regulating treatments.
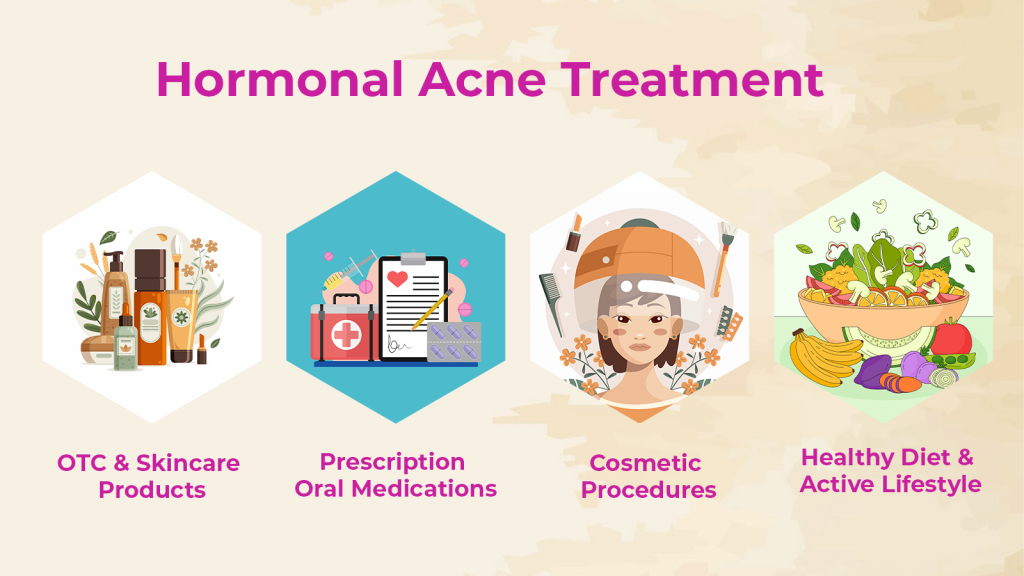
The treatment of adult acne involves a combination of natural and medical fixes. While using topical creams may reduce sebum production and inflammation of lesions, it is essential to fix hormonal fluctuations from within as well.
Take a look at the following hormonal acne remedies that a professional may recommend based on the severity of the acne:
Retinoids belong to the family of Vitamin A derivatives, which can help treat skin conditions like psoriasis and acne, reduce the appearance of signs of ageing, and improve skin texture.
Mild to moderate acne can be treated well with these OTC retinoids:
While these retinoids are easily available at pharmacies, it is paramount to consult with a doctor before using them to avoid potential skin complications. Also, these hormonal acne creams can come in the form of gel or cream, and should be applied strictly in the evening.
Commonly used skincare actives like salicylic acid and benzoyl peroxide are other relevant topical hormonal acne treatments. One can use a foaming salicylic acid face wash daily twice in the morning and evening, while using a benzoyl peroxide gel in the evening after cleansing, followed by a non-comedogenic face cream.
Oral antibiotics, including doxycycline, tetracycline and minocycline, can help reduce the inflammation and redness caused by pustule or cystic acne. Another potent oral medication for preventing and controlling hormonal acne includes isotretinoin.
Isotretinoin (Accutane) is a strong retinoid which is often suggested as a last-resort treatment option by professionals for patients with moderate to severe and persistent hormonal cystic acne. It functions by controlling sebum production, reducing inflammation and preventing clogging of hair follicles.
Anti-androgen drugs like spironolactone stabilise the hormone receptors, regulating the androgen count in females. This prevents the hormone from affecting hair follicles and increasing sebum.
Contraceptive (birth control) pills containing ethinyl estradiol, norethindrone, drospirenone and norgestimate together can block the androgen hormone, causing adult acne, and especially benefit women during the ovulation phase in their menstrual cycle.
Other anti-androgen medications include ingredients like cyproterone and metformin, which can help regulate hormonal fluctuations and control acne.
A non-invasive, dermatological acne treatment that uses a safe chemical solution chemically formulated to exfoliate the skin on a deeper level. This exfoliation helps unclog pores, hence preventing breakouts and even ensuring a smoother, clearer complexion. Professional-grade chemical peels also relieve patients from acne inflammation.
Laser treatment is an ideal choice for individuals seeking drug-free treatment. It works by targeting sebum glands, shrinking them and reducing excess oil, hence preventing clogging of pores. It also helps calm hormonal acne-related inflammation and further reduces the appearance of post-acne dark spots.
Hormonal acne diet involves specific food choices that can help reduce acne-related inflammation, manage insulin spikes, and stabilise blood sugar levels. Let’s take a look at the food that one can include to regulate hormonal fluctuations:
Berries, nuts, sardines, salmon, chia seeds, walnuts, flaxseeds and leafy greens reduce oxidative stress and promote skin health.
Opt for brown rice, whole wheat and quinoa over refined carbs to avoid an insulin spike. Similarly, choose good sources of fibre like beans and legumes to control blood sugar.
Almond milk, soy milk, and oat milk are excellent alternatives to cow milk and can help prevent hormonal acne flare-ups.
Apples, plums, papayas, and grapes should be included in the diet to limit the consumption of sugary fruits.
Besan chila, chicken salad, or an oats bowl in the morning can help regulate blood sugar and contribute to healthy skin.
If hormonal acne persists even after using topical creams, following a healthy lifestyle and consuming a hormonal acne-friendly diet, seek professional advice from a reputable dermatologist. At Wizderm, our expert team of doctors offer a detailed skin analysis, helping you understand the root causes of acne and offer appropriate and customised treatment plans. Book your consultation today at Wizderm Skin and Hair Clinic!
Yes, hormonal acne is also called ‘adult acne’, as it mainly affects men and women between the ages of 20 and 50, specifically after hitting puberty.
No, hormonal acne can show up on one’s face (lower cheeks, chin and jawline), shoulders, back and even chest.
While stress is one of the major triggering factors of hormonal acne, flare-ups can also be caused due to an increase in androgen hormones in the body, a diet rich in high glycemic foods and dairy, and a lack of involvement in physical activity.
The speed at which outcomes show up depends on the individual’s skin type, severity of the acne lesions and the treatment type. However, topical treatments can take up to 6 – 8 weeks to show visible changes with consistent use, while clinical procedures, such as chemical peels, can yield results much faster, often in just a few sessions.
Yes, hormonal acne can affect both men and women, and treatments are available for both genders.
Absolutely not! Popping or picking at the hormonal acne cysts can cause transfer of the bacteria or oil across the nearby areas and lead to further breakouts.
Yes, dairy and sugar can worsen hormonal acne by increasing androgen and insulin levels, thereby boosting sebum production and inflammation. This, therefore, leads to more breakouts.
Yes, it is very likely to treat mild to moderate hormonal acne with only topical retinoids, chemical peels, healthy lifestyle habits, and dietary tweaks, eliminating the need to consume medications.
Yes, birth control pills regulate the androgen hormones that trigger acne in women, reducing breakouts and inflammation. However, one must strictly consult with a doctor about its usage, especially if the acne condition is moderate to severe.
Registered Office
Wizderm Speciality Skin & Hair Clinic 1/503, Gariahat Road, Jodhpur Park, Kolkata, West Bengal 700068
Mon - Sat: 10 AM - 8 PM
© 2026 Wizderm Speciality Skin & Hair Clinic. All rights reserved.
Crafted with by Auraveni Solutions.
Stay updated with expert tips, latest treatments, and exclusive offers. Subscribe to Wizderm's newsletter for healthy, glowing skin and hair!